Infusion services for military active duty, families, retirees and veterans
For your TRICARE® and VA CCN infusion care experience, we’ve got you covered

Our broad portfolio and unmatched access to drug manufacturers give patients access to virtually any therapy across multiple specialties and disease states — including new FDA-approved medications.
Our nationwide network of nurses and pharmacies have the capability to support therapy needs for all military veterans and TRICARE beneficiaries, no matter the situation:
• Continuing to work
• Deploying
• Transitioning to a new duty station or temporary duty
• Going on convalescent leave
• Living in base housing/barracks

• IV Antibiotics
• Enteral Nutrition
• Parenteral Nutrition
• Chronic Inflammatory Disorders
• Immunoglobulin
• Bleeding Disorders
• Women’s Health
• Neurological Disorders
• Specialized Therapies

Streamlining and removing administrative burdens
Our government program focused patient registration team verifies TRICARE and VA CCN eligibility and authorization for all referred TRICARE enrollees and veterans. This saves prescriber’s time, so patients can start treatments sooner.
- Enrolled as a participating provider in Medicare and Medicaid as well as coordinated care for TRICARE for Life beneficiaries
- Cost shares calculated according to TRICARE policy rules and reimbursement so eligible beneficiaries know what they are responsible for paying
Option Care Health is the only national infusion provider in-network with every major health plan, including:
- TRICARE East – Humana Military
- TRICARE West – HealthNet Federal Services
- TRICARE Express Scripts®
- VA CCN Optum®/ TriWest®
- CHAMPVA
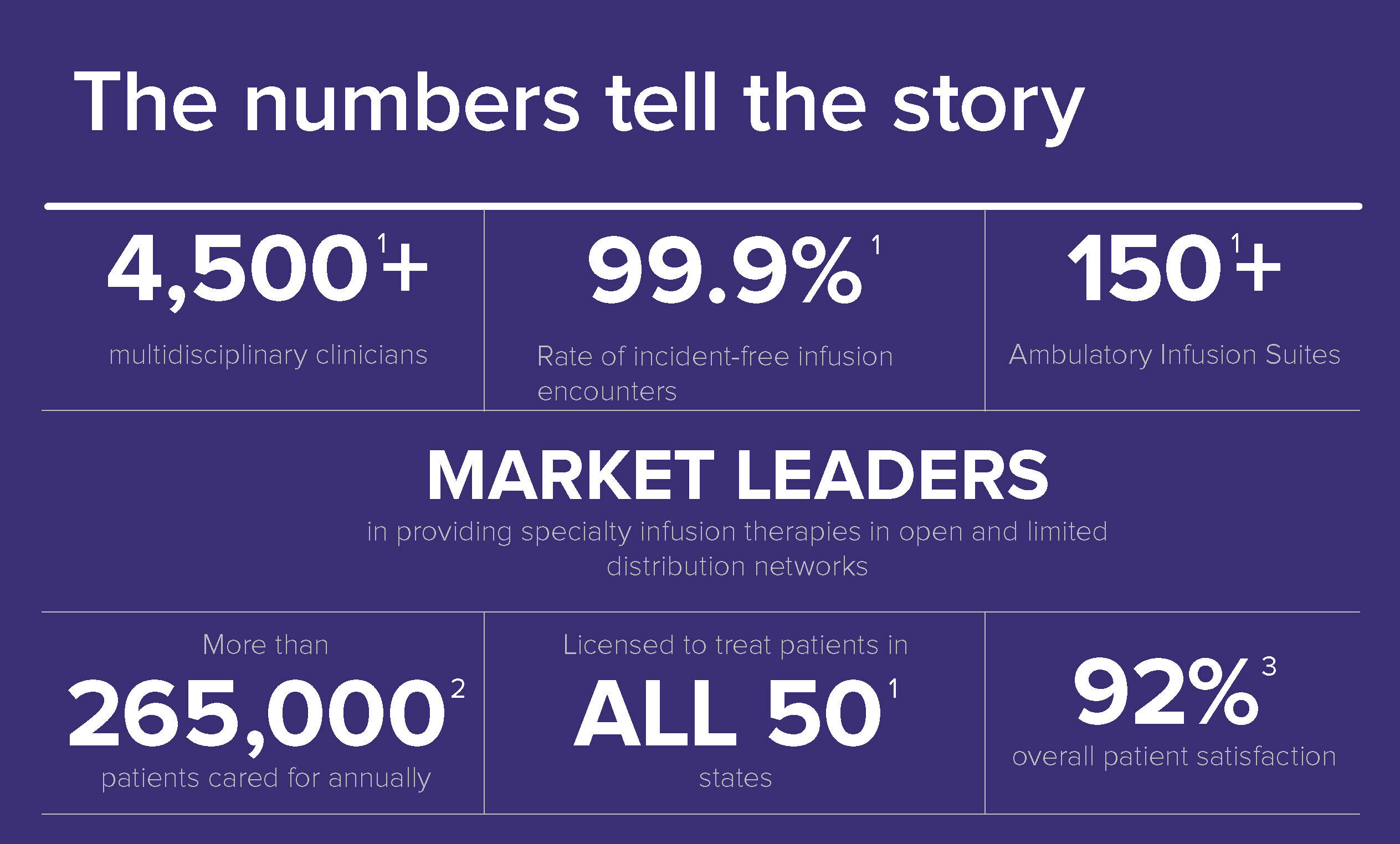
References: 1. Data on file, Option Care Health. 2. January-December 2022, total Option Care Health unique patients serviced. 3. January-December 2022 patient satisfaction data.
Survey of 25,918 patients.
